|
It has been postulated that LAM is released from metabolically active or degrading mycobacterial organisms into the serum, with subsequent filtration by the kidneys, passing into the urine where it can be detected by enzyme-linked immunosorbent assay (ELISA). In addition to host factors which may affect LAM detection such as immune status, the quantitative expression of LAM on the mycobacterial surface has also been shown to be strain dependent. A simple, low-cost, point-of care version of this assay has been shown to have considerable utility when screening for TB prior to antiretroviral therapy. However, sensitivity of the assay has been reported to be increased in HIV-TB co-infected patients with advanced immune suppression and also in those with high TB bacillary burden. Urine LAM testing has shown markedly variable diagnostic accuracy for TB in field studies with a generally low sensitivity. LAM antigen is a 19,000 (± 8,500) daltons sized lipopolysaccharide which can be recovered in large quantities from Mycobacterium tuberculosis ( Mtb) cultures, and is detectable in serum, sputum and urine in a wide variety of tuberculosis (TB) clinical settings. Both LAM antigen and anti-LAM antibody may be found aggregated in circulating antibody-antigen immune complexes. The detection of anti-LAM antibodies has been proposed for diagnosis of active tuberculosis. LAM is also highly immunogenic and anti-LAM antibodies are produced during mycobacterial infection. LAM is present at the cell surface where it can readily interact with host receptors and act as an immunomodulator. Lipoarabinomannan (LAM), a major lipopolysaccharide component of the cell wall of the genus Mycobacterium and related actinomyces, was first characterised in the 1980's. The strong association of urine LAM with mycobacteriuria is a new finding, indicating frequent TB involvement of the renal tract in advanced HIV infection. Urinary LAM was related to host immune factors, was unrelated to Mtb strain and declined steadily after an initial 2 weeks of TB treatment. Mycobacteriuria was found in 15/32 (46.9%) of LAM positive patients and in none of the LAM negative controls. The sensitivity of LAM for TB in HIV-infected patients with CD4 counts of ≥ 200, 100-199, 50-99, and < 50 cells/μl, was 15.2%, 32%, 42.9%, and 69.2% respectively. 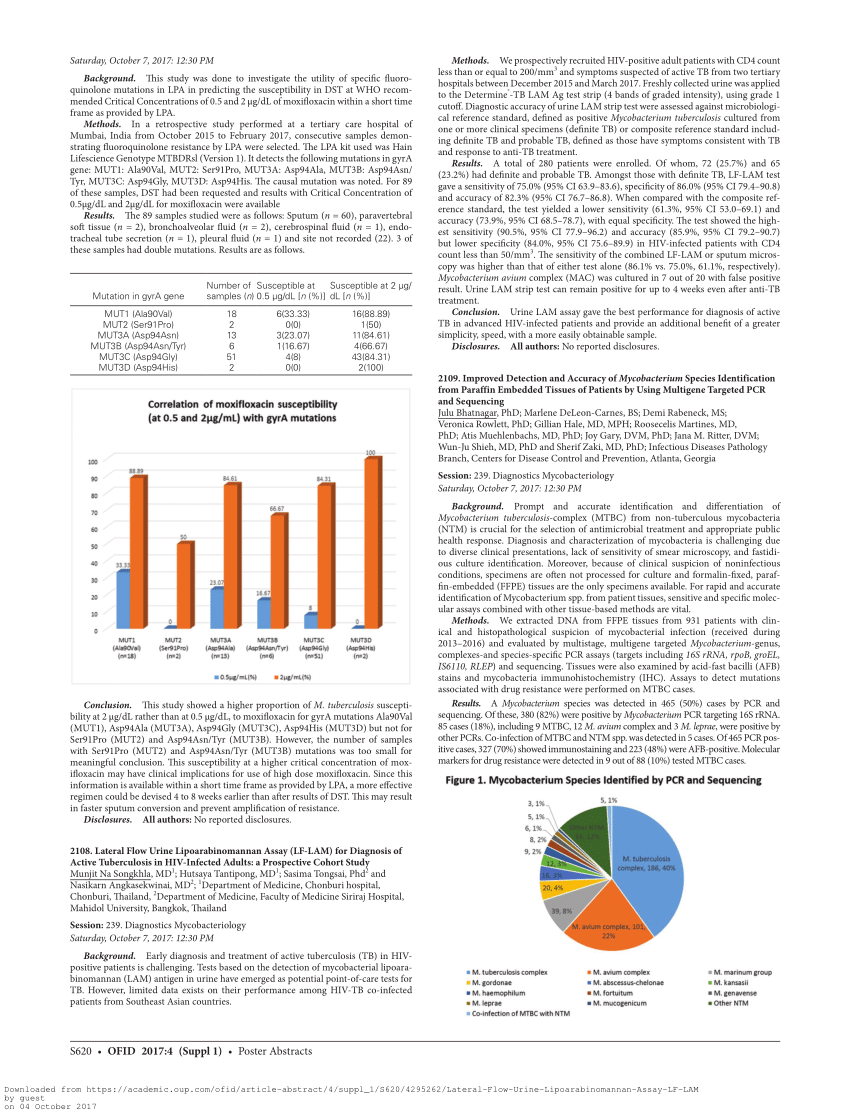
LAM was associated with positive sputum smear and culture status, HIV infection and low CD4 cell counts but not proteinuria, RFLP strain or TB treatment outcome. Median optical density and proportion testing LAM positive remained unchanged during 2 weeks of treatment and then declined over 24 weeks. 
Resultsģ2/199 (16.1%) of patients tested LAM-ELISA positive. 
Sputum TB isolates were characterised by IS 61110-based restriction fragment length polymorphism (RFLP) and urines were tested for mycobacteriuria by Xpert ® MTB/RIF assay. LAM-ELISA assay testing, sputum smear and culture status, HIV status, CD4 cell count, proteinuria and TB outcomes were prospectively determined in adults diagnosed with TB and commencing TB treatment at a South African township TB clinic. We therefore explored pathogen and host factors potentially impacting LAM detection. However, the LAM-ELISA assay has demonstrated variable sensitivity in diagnosing TB in diverse clinical populations. Detection of lipoarabinomannan (LAM), a Mycobacterium tuberculosis ( Mtb) cell wall antigen, is a potentially attractive diagnostic.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
